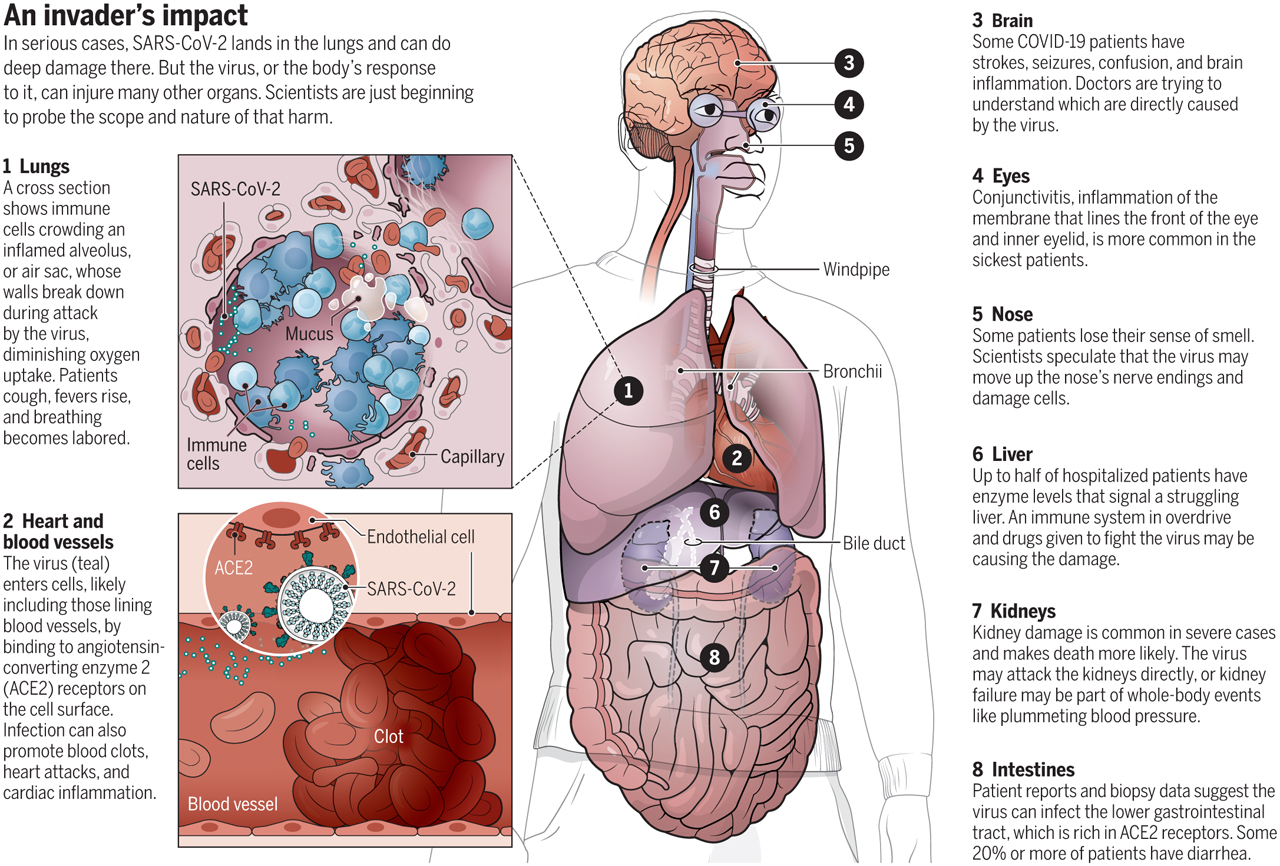
image by V Altounian in Science magazine showing some of the early discoveries about the widespread and serious effects of CoVid-19 on the body (other effects, and unique effects on some infected children, have been found since this report)
I said my previous post on CoVid-19 would likely be my last, at least for this “wave” of the disease, but I thought it might be useful to summarize what we now know (which is still pathetically little), and what we still don’t know (mostly everything) about this disease, as we head into the summer months. I’ll avoid proffering any advice, for a ton of reasons, but the common sense approaches to take at this juncture, erring on the side of caution, are pretty obvious.
What we think we know at this stage:
- The Infection Fatality Rate (proportion of those infected, even if asymptomatic, who subsequently die — the IFR), and the Case Fatality Rate (proportion of those testing positive for the disease who have symptoms and subsequently die — the CFR), are probably about 0.6% and 1.0% respectively. This is many times higher than “normal” flu rates, but mercifully much less than those of some other viruses and coronaviruses in particular. Pre-peer review studies suggesting a much lower IFR have been largely discredited by the epidemiological community (the most popular of these low-ball studies was issued by a researcher who a few months ago was predicting only about 10,000 US deaths from CoVid-19). But due to inadequate testing, these rates are still only approximate.
- The actual number of CoVid-19 deaths in developed countries, based on extensive “excess deaths” studies, is likely to be and will likely continue to be about 1.5x officially reported numbers, mostly due to people dying from CoVid-19 at home without ever being tested, and uncertainty in cases of comorbidity. The multiplier will be higher, in some cases much higher, in places with poor reporting and testing systems. Worldwide, a very rough estimate would be that actual first wave deaths have been and will continue to be about 2-3x officially reported numbers, which would produce an actual death toll by end of summer of about two million people (and reported deaths of just under one million).
- If this IFR and excess deaths multiplier are close to correct, then by the end of the summer about 4-5% of the global population will have been infected; the rest will remain highly vulnerable to CoVid-19 infection in the fall or in later waves, in the absence of a safe and reliable vaccine, particularly as social distancing and other measures are relaxed or are no longer diligently followed. The infected rates by summer’s end will vary hugely — likely around 6% in Canada, 12% in the US, 15% in much of Europe, even higher rates in much of Latin America, perhaps 2% in India and much of Africa and the Mideast, and 0.1% in China and some other Australasian nations. None will reach “herd immunity” levels.
- We are utterly unprepared in most of the world for the large-scale testing, contact tracing and isolation that would be needed to avoid surges in infections and deaths in the fall and thereafter. As a result, we are almost certainly going to have to get used to the severely restrictive social distancing, recurring shut-downs, and other economically- and socially-destructive measures that we have struggled with in recent months. Depending on vaccine success, virus mutation and wave severity, that could continue into next year and possibly the year beyond.
- Based on serology testing, all age groups seem to be roughly equally susceptible to infection, but the rate of symptoms, hospitalization and death (the IFR) varies enormously by age and health (those >65 have an IFR an order of magnitude larger than average, and those <29 have an IFR an order of magnitude lower). The notable exception is that serology testing shows, surprisingly, that a relatively smaller proportion of seniors have been infected (though their IFR is by far the highest). There are several possible reasons for this — they could be being more careful due to their greater vulnerability, or they may have natural immunity due to recent exposure to other similar coronaviruses, or there may be other reasons. We don’t know. But it does mean that the most vulnerable age group actually has the lowest rate of infection (and hence future immunity) to date, which is concerning.
What we really don’t know at all at this point:
- The biggest and most important unknown is that we still have no idea how this virus kills us, and what its long-term effects are. Tests of people who have tested positive for antibodies (serology tests) but who were asymptomatic or suffered only minor symptoms have found substantial evidence of significant lung and other organ damage, whose cause and future prognosis are completely unknown. This disease affects not only the lungs, but also the heart, brain, nervous system, kidneys and other organs in ways we are only just beginning to understand. You may be completely asymptomatic or seemly unharmed by infection, and yet have already suffered damage that will, later on, lead to chronic and debilitating illness or premature death.
- We have no idea how effectively or for how long immunity will be conferred on those infected. Early research suggests that CoVid-19 antibodies drop off quickly in the weeks and months after infection, though some immunity seems to be present in some infected people even with no measurable antibodies. This makes the challenge of developing a safe, effective and affordable vaccine, and the challenge of re-administering it when it wears off, even more difficult.
- Of course, we have no idea when such a vaccine may be available. It is likely that the first vaccines will be less than fully effective and it will take additional time to fine tune them to the ever-evolving strains of the virus. There are already several different strains of the virus, with apparently different IFRs.
- We have no idea how this virus will mutate, and if it will mutate to a less lethal form or, like the 1918 pandemic virus, into a much more lethal form.
- We have no idea what, if any, pattern of seasonality this virus will present, and hence when to be most alert for new outbreaks.
- Currently reported cases are spiking in many jurisdictions that have relaxed social distancing, notably in the US. We have no idea to what degree this is due to increased testing versus increasingly risky behaviour; it is likely a combination of both, along with other, unknown factors. We do know that average age of those being tested, and of those testing positive, are skewing sharply lower than during the first months of the disease. We don’t know why, though the high vulnerability of older people (who were most likely to be symptomatic and hence to be tested earlier) is certainly a factor.
- As a result, we have no idea to what extent this increase in cases will translate into increased deaths in the weeks to come (there is a lag of about 3 weeks on average between disease onset and death in fatal cases). There is already evidence of increased hospitalizations, but reported deaths so far continue to trend downwards. And with younger cases, we should expect lower mortality rates. No one knows, and it will take until the end of July, or longer, to find out.
- The IHME (UW model) now predicts an upswing in deaths starting slowly in September and then rising sharply by the beginning of October in the US, Latin America, UK, Italy, Germany and Russia (their model excludes much of Africa and Asia). At this stage they are not making any projections past then, because everything depends on the behaviours of both governments and citizens especially in the most-affected countries. Isolation fatigue could play a significant role, though IHME has factored into their projections expected shutdowns where they forecast hospitals will exceed their ICU capacity by October 1st. It is worth noting that in its projections IHME more or less ignores the officially reported case counts as being highly unreliable and incomplete, and instead uses its own model. According to that model, actual new infections have been about 10x the reported case numbers, and actually peaked in the US in late March (working backwards from the smoothed peak in reported deaths there in mid-April), and have sharply dropped since then and will continue to drop slowly until schools reopen in late summer. This tells a very different story from the “official” new infections data showing new cases in the US at record highs in late June*. If IHME are wrong in this assumption, their death forecasts could therefore be wildly off. (Their forecasts for Europe are based on the same assumptions, with slightly earlier infection peak dates.)
- And of course, we don’t know how our adaptation to this virus is going to affect national economies and the global economy. Stock markets are, ludicrously, at or near record highs, which demonstrates that they are no longer useful measures of our economic health, if they ever were. Unemployment remains historically high, and there’s a strong resistance from many to a return to business as (obscenely unequally) usual. At the same time, new data shows that while incomes for most have plummeted, consumer spending is returning to near “normal”; people are just going, endlessly, deeper and deeper into debt. Will CoVid-19 create the inequality and precarity “flash point” to produce long-term social unrest and political upheaval? And even if it does, will that be enough to collapse an economy we all depend so heavily on? And what would all that mean for the trajectory of the pandemic? No one knows.
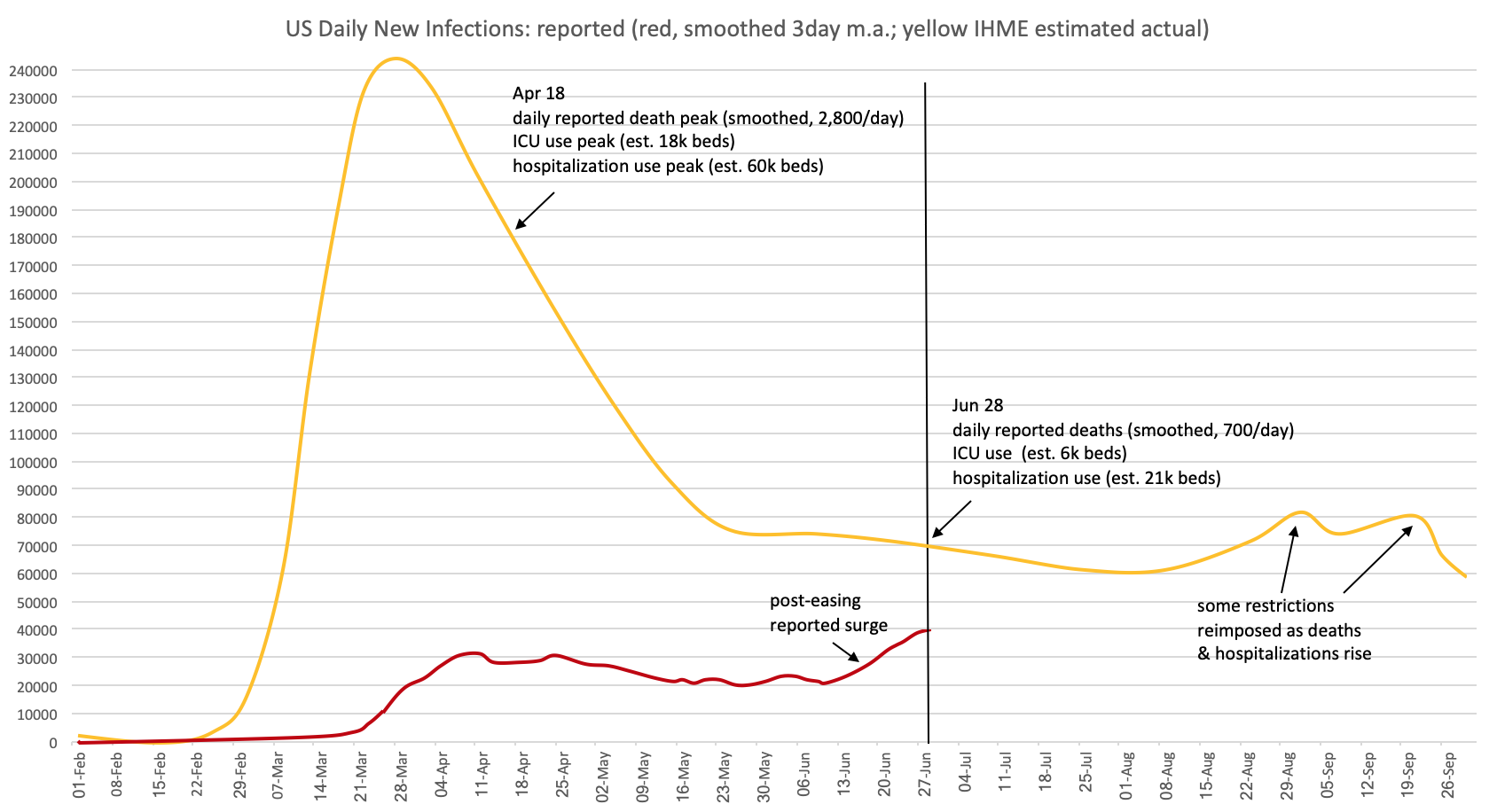
*Here are the smoothed (moving average) data for reported new daily US cases (red), compared to the estimated actual numbers of new daily cases (yellow) that IHME uses in its forecasts. While the late-June “surge” in reported cases looks alarming, it may just reflect that finally a larger proportion of actual new infections are being tested and reported. As noted above, that doesn’t mean reopening is wise: 70,000 new cases a day is still dangerously high and the projections could change quickly if social distancing, event-size and business opening rules are eased too quickly or not followed. And 70,000 new infections a day means a million Americans will be infectious to others each day through the summer.
PS: June 29 addendum: just in, from Michael Greger on CoVid-19’s apparent effect on the immune system:
[The cytokine storm reaction of some of those infected with COVID-19 who have healthy immune systems] has led some to consider immunosuppression [eg steroids] as a treatment for severe COVID-19, but of course immunosuppression for hyperinflammation in COVID-19 might be a double-edged sword. So, when you see that broccoli sprouts can whip up natural killer cell activity within two days, is that a good thing or a bad thing for COVID-19? It was good for seasonal flu, but who knows with this new coronavirus.
Young children have relatively immature immune systems, and normally suffer disproportionally from viral infections such as the flu––but not, apparently, from COVID-19, or SARS or MERS, for that matter, the other two deadly coronaviruses. It’s interesting; one theory as to why children seem protected suggests that greater pre-existing exposure to common-cold coronaviruses offers kids some cross-protection against the new virus. But ironically, a competing theory suggests it’s their lack of exposure to similar viruses that’s safeguarding them. There’s a phenomenon known as ADE, antibody-dependent enhancement, a phenomenon first described more than 50 years ago. In most cases, the antibodies our bodies make to target pathogens neutralize them or, at the very least, tag the invaders for removal. Sometimes, though, antibodies can actually facilitate viral infection and exacerbate disease.
This may be the case with SARS, where antibodies generated against the viral spike proteins were sometimes found to promote infection. In monkeys, an experimental SARS vaccine resulted in aggravated lung damage. Now, vaccine developers are well aware of this phenomenon, and would work to ensure any commercial vaccine would be free from this failing, but it has been used to venture a guess to account for the unusual age distribution of severe COVID-19 cases.
Perhaps similar coronaviruses circulated silently decades ago, and those old enough to have been exposed to them are now experiencing exaggerated responses to COVID-19. But young people never saw them, so they don’t get the over-reaction. I’m not suggesting this speculation is true. I just use it to illustrate the complexity of our immune interactions. Viruses attack, we counterattack, and then viruses sometimes evolve to use our own counterattack in their favor.




