Forecasts April 9th, 2020 (shortly after this article was first written):
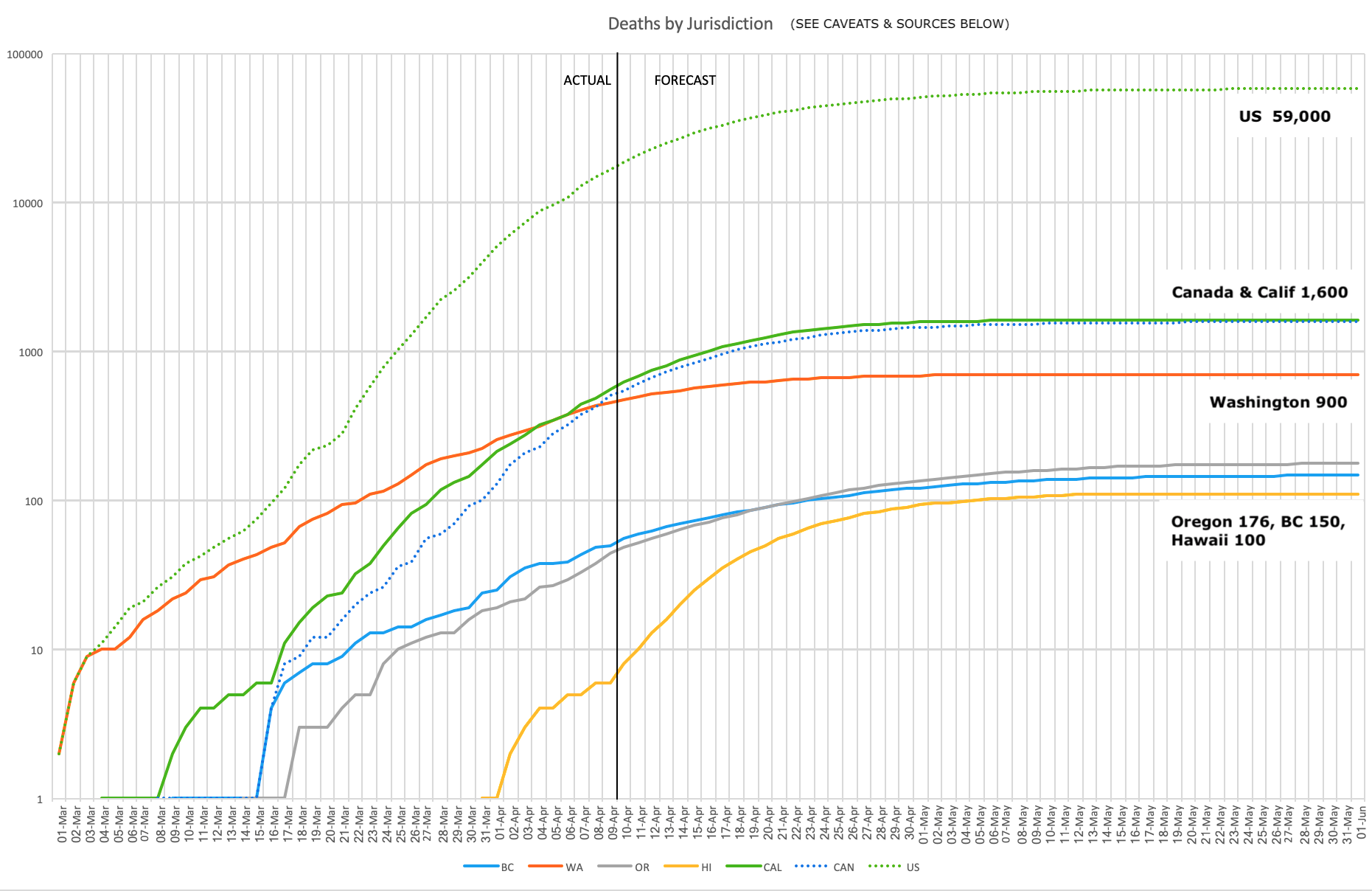
[EDIT] Updated Forecasts May 4th, 2020:
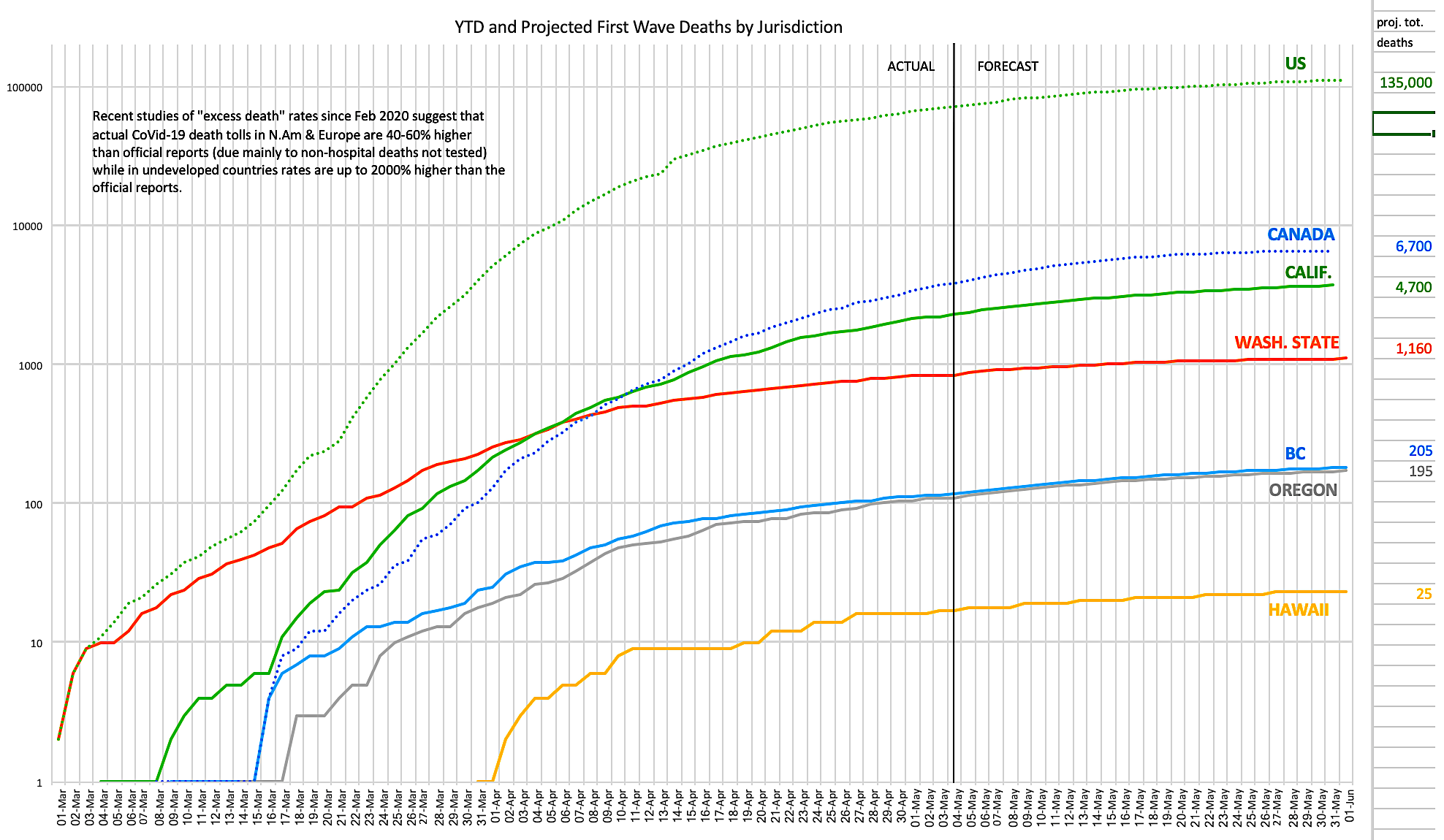
Current CoVid-19 deaths for North America West Coast jurisdictions to [EDITS: updated to April 9th & May 4th] per the nCoVid2019 Dashboard, and projected most likely (95% confidence intervals: +/- 50%) total deaths to the end of this wave of the pandemic for each jurisdiction per U of Washington IHME projections as at [EDITS updated to April 7th and May 1st]. Interpolations of this data for Canadian jurisdictions in the top chart are mine. Click on images for larger versions. Download the latest version of this Excel chart and data. (I plan to keep it current until at least June 1.)
Caveat 1: I am not an expert in this subject, and these are only my wild informed guesses, subject to drastic future change and possibly great retroactive embarrassment. But I thought I’d try to summarize how it looks to me at this pivotal point, based on my experience and research.
Caveat 2: The above IHME April 7th projections are much more optimistic than just a week ago (1/3 fewer projected total deaths); [EDIT] the updated May 1st projections are nearly twice what was projected just a week earlier. These projections assume no further waves and no slackening of social distancing until either (1) resources exist to do exhaustive ongoing testing, or (2) an effective vaccine is fully implemented. The top chart early predictions have already been exceeded, and in my opinion death totals 40-60% higher than even the upward-revised (lower chart) projections are likely once unexplained excess deaths have been factored in.
The most important things to keep in mind right now IMO:
|
LEARNING FROM PAST PANDEMICS
When I worked 12 years ago with the Ministry of Health with a special group hired to learn the lessons of SARS so there would be no repetition of the mistakes made then, we studied the epidemiology not only of SARS (CoV-1) but of various bird flus (H5N1, H7N9), swine flus (H1N1), and the 1918 pandemic (“Spanish flu”, also an H1N1).
What was so remarkable about this work is that most of what we would ideally like to know/learn about these diseases we could not learn, for a number of reasons — mostly about how incredibly little we really understand viruses and how they proliferate, but also because the history is still unclear. You would think, for example, that by now we would know where the 1918 pandemic arose, but we remain utterly clueless, with at least 3 major theories, all of them somewhat suspect.
We also can’t yet agree on how many died from the 1918 virus, with estimates varying by more than an order of magnitude.
Nevertheless, there is much to learn from that pandemic, and I’d commend this New Yorker video to you — an interview with John Barry, a writer who’s spent much of his life studying it.
Some things that we did learn, that now seem to have become lost in the shuffle:
- Flu pandemics come in waves. The severest wave in 1918 was the second, not the first. And it wasn’t (so much) because people got complacent and eased restrictions when the first wave abated; it was because viruses can mutate incredibly quickly, and the second wave arose from a much, much more virulent strain.
- Unlike most flu viruses, including the first 1918 wave virus, the second wave 1918 mutation struck almost entirely young people. It did this by inciting what is called a cytokine storm in the bodies of its victims. It wasn’t the virus or any side effects of the virus (like pneumonia) that killed the second wave victims, it was the victims’ own immune systems. So those with autoimmune disorders (hyperactive immune systems) were devastated, while those with suppressed immune systems were almost entirely spared (fewer than 1% of second wave victims were over 65).
- There were several waves of the 1918 virus after the second one, but a peculiar paradox made them much milder: The second mutation essentially ran short of available hosts, and had to mutate to survive. The second mutation was simply too potent for its own good, and essentially eradicated itself by mutating into a much milder form.
MODELS OF WHAT TO DO NEXT TIME
The economic impact of this virus, due to our unpreparedness for it, will be staggering. There is a significant risk of a long and deep economic depression (more on that in a future article). But this didn’t have to be.
Some jurisdictions have been largely spared both the health and economic costs of this virus, notably Taiwan. Lessons from their experience and preparedness:
- A process must be in place to enable rapid and repeat testing of every citizen, to quickly isolate the disease. The cost of being ready with swabs, masks, sanitizers, protective shields and test equipment pales in comparison with nationwide economic shutdowns, and such shutdowns are needed only because we have no idea who has the virus now. It is very likely that actual positive cases (if we had the tools to test for them) would be about an order of magnitude (10x) the current “official” figures, which have resulted from testing only those who already exhibit strong symptoms.
- In Taiwan, spreading fake news, hoarding, price-gouging and other actions that exploit and inflame the situation are indictable offences and considered shameful, not shrewd, behaviours. There, businesses and schools and restaurants are re-opened and life is nearly normal, and there’s been very little effect on the national economy.
- The town of Vo, in Italy, had the luxury of having the equipment and political will to test and retest every one of its 3,300 residents and isolate those who tested positive, even if asymptomatic. Their experience is a model for every community in the world to follow, if we’re willing to learn from it.
PREVENTING PANDEMICS IN THE FIRST PLACE
While the above models can dramatically mitigate the impact of pandemics when they first occur, it would be even better if we were to prevent them happening in the first place. When Dr Michael Gregor was working in epidemiology a decade ago, he published his findings on the history of human pandemics and their causes. He revealed that virus transmission to humans only became possible with the domestication of animals 10,000 years ago, and all known human viral infections (poxes etc) have their origin in domesticated animals or the consumption of bushmeat — without it there is no way for viruses to move from their endemic animal hosts to humans who have no immunity to them (hence leading to pandemics).
Two centuries ago pandemics became more prevalent again, commensurate with the intensification of “industrial” agriculture. Then with the development of vaccines, infectious diseases were almost eradicated from the planet by the 1970s, causing some health leaders to predict that such diseases would never again cause pandemics.
But then suddenly there was a third huge upswing in novel infectious diseases, starting just 30 years ago. This corresponded with the order-of-magnitude increase in CAFEs (factory farming) of both domesticated and “exotic” birds and mammals for human food. Pangolins may the source of SARS CoV-2 (the current coronavirus that is expressed as CoVid-19).
There is nervous laughter around the room when Michael says, at the end of the 2009 presentation linked above, that “we could well face a situation in the near future where every American might have to shelter in place for as much as three months to prevent spread of a global lethal pandemic”.
It is to be hoped that, along with all the other learnings from this current horrible outbreak, we take to heart that only by completely ending the three sources of the recent upsurge in pandemic risks — (1) disturbance of the last wild places on the planet that harbour viruses for which there is no natural human immunity, (2) the bushmeat trade including domestication of “exotic” species for food, and (3) factory farming — will there be any chance that situations like that we are currently facing will not become increasingly frequent and dangerous.
But I would be surprised if there’s even an acknowledgement of this cause, outside an increasingly censored and silenced scientific and medical community.
MORE INFO
- The charts at the top of this post came from IHME projections, and the underlying data is available here if you want to make your own or track the accuracy of them. They’re especially useful if you’re in a state that will likely face severe hospital bed, ICU or ventilator shortages and hence excess preventable deaths: New York, New Jersey, Connecticut, Michigan, Louisiana, Missouri, Nevada, Vermont and Massachusetts.
- The IHME used in its modelling information on other countries’ death rates after the number of deaths and infections reached a certain base level (“trajectories”). Our World in Data is maintaining excellent charts on trajectories. So is John Burn-Murdoch for the UK Financial Times.
- The data suggest that the mortality rate, on average, is converging on a rate of 1% of those infected [EDIT: Update May 4th: mortality rate now looks to be closer to 0.2-0.5%]. But the number of people testing positive (due to drastically limited testing stemming from unavailability of test kits and testing resources) is wildly underestimated (the actual number of those who would be testing positive if everyone had been tested is likely 8-20x the reported numbers). That means, if the projections pan out, that only 1.5-2.5% of North Americans would actually test positive at some point during the current wave, if the test were available. Without social distancing, it was estimated that 25-50% of the population would eventually contract the disease. This is the power of social distancing: It is almost certainly saving tens of millions of lives worldwide. It is these tens of millions of lives saved that we must weigh against the horrific economic cost of this pandemic, which is only beginning to emerge.
WHAT TO DO NOW
- Depends on your situation, of course. If you’re needed in the food, health care and other essential fields, thank you for continuing to do what you do. If you have things you can give away safely to people who would benefit from them, of course please do so. If you’re in financial peril as a result of the economic shutdown, the resources available to help differ in each jurisdiction.
- [Edit: Added Mar 30] If you can, please get involved in the various “mutual aid networks” that have sprung up since the pandemic started. Here’s a summary of how they work. Here’s a US directory. Here’s a global directory. Most communities have something like this going for peer-to-peer support, as governments are often overwhelmed, too distant, underprepared or in some cases in denial. [Thanks to Kevin Jones for reminding me about this.]
- If you’re like most of us, the next few weeks especially will bring a lot of anxiety, and feelings of anger, being trapped, feeling shameful etc. These are all manifestations of grief (thanks to Maureen Nicholson for the link). There are many online resources on coping psychologically with this. Here’s one (thanks to John Graham for the link) that I find useful.
- Keep up the pressure to sustain social distancing on your government, if it’s dragging its heels or proposing to relax the rules. Here are the worst offenders globally. Likewise if your peers are flaunting the rules (the link above also has a tab on citizen behaviours, which largely parallels their governments’). Millions of lives are at stake.
- Limit your time on useless social media and other media that are mostly or entirely unsupported opinion, useless information and misinformation. If it’s not actionable, and doesn’t give you any sense of comfort that you’re doing the right things by being overcautious, and that it’s going to be OK, then there’s really no benefit in reading it.
And for the vast majority of us, it is going to be OK.
Next articles here will be on the economic fallout, which is likely to be longer and deeper than the health impact, but was overdue to happen anyway, and on why this horrible event may be a useful wake-up call that might get us started addressing some of the more profound and permanent challenges ahead.
Stay safe, everyone.





Peter Kaminski just pointed me to another great site where you can put in your own assumptions for any country in the world and it will compute infections and deaths: https://whyimstayinghome.com/?lang=en
But I’d recommend using the Advanced Setting to set mortality rate to 1.0% instead of their default 0.5%, since I think that’s what IHME used.
For me it hasn’t been excessively disruptive so far – it’s a pleasant break from the hectic behaviour in the suburban world. I’m fortunate that I can work remotely and I’ve been spared the draining experience of having to go into an unpleasant office. Where I might be accused of being a bit of a hermit in my usual life, this has now become helpful. To be honest I think people often go out for the sake of it just when they’re bored.
I’m pessimistic as to whether anything will be learned. I’m also wondering if the main damage to “the economy” is rich people not being able to be as rich as they were hoping this year. I realise poor people are the first to get dropped in “cost savings” but when some public figure talks about “the economy” you know they don’t mean people who have no real stake in it and have to scrape around to survive.
Like you say most of us will be ok. At the back of my mind I wonder what would happen in a real crisis where food supply actually is a problem and scarcity hasn’t been manufactured by foolish behaviour.
I am tracking the rise of mutual aid groups across the country and I am seeing them move into a phase of not just cooperation; one off mask making projects but rapid open source ventilator and intubation screened masks, integration with health care system supply chains, and other forms where they are becoming partly institutionalized and likely to last past the summer to become part of the citizen driven landscape. This is creating a wave of interdependence that will change societal attitudes toward property and alter our sense of ourselves as isolated individuals but can build mutuality as a key to our collective survival. That article will be out this week.
This is the first article covering the interdependence beat https://symbioticfund.wordpress.com/
Hey Dave,
Wanted to acknowledge this body does seem to experience some calm from the suggestion of radical non-duality with regard to this Covid-19 thing. As Jim Newman said “The dog shit on the ground that you just stepped in is saying ‘this is all there is, this is fulfillment’ “. Seems it would follow that “The coronavirus is saying ‘this is all there is, this is fulfillment’ “. In other words thanks for sharing all the links you have on radical non-duality.
Best,
David
Thanks David. It works for me a bit — perhaps more than I realize — but I don’t seem to have much control over the anxiety when it happens. Tim/Jim/Tony make the point that the self/sense of separation isn’t just a thought, it’s an embodied energy. There seems to be a kind of mind/body feedback loop that keeps the self activated, what Eckhart Tolle calls “egoic mind/pain body”. But I think it’s asking a lot of people to even begin to contemplate that ‘we’, apparent human characters, would be perfectly functional and actually better off without our illusory conscious selves. Not to mention that we have no free will. Them’s fightin’ words.
Dave, I really appreciate a sober mind in these very scary times which are coming upon the world. However, I have to bring my own angle to this. Have you ever read Douglas Adams’ “Hitchhiker’s Guide to the Galaxy?” It was a favourite book of mine as a kid. I especially enjoyed the little subplot in the first chapter or three. Today, I feel like the woman in the pub in that story, who comes up with the answer to save the world, and despite that, the Vogons aim their beams at planet Earth and destroy it, with only Arthur Dent and his buddy going off to explore the universe.
My stepmom who my Dad married when I was in seventh grade was a respiratory therapist. I, myself, had struggled with hay fever my whole life. And after a few weeks of thinking about this, and watching these horrifying events unfold, I honestly believe I have a starting point with which people could stop the death.
It has to do with a perspective shift from “How do I avoid the virus?” to “How do I recover from a respiratory illness?”